Is your staff trained in intermittent auscultation?
Self-paced, simulation-based education from Step Up Together® is here.
Primary Maternity Care and the Institute for Perinatal Quality Improvement (PQI) have partnered to offer a special Step Up Together edition of Intermittent Auscultation Simulation-Based Education—a virtual course designed for nurses, midwives, paramedics, physicians, and other clinical team members committed to providing safe, patient-centered care during labor.
Primary Maternity Care and the Institute for Perinatal Quality Improvement (PQI) have partnered to offer a special Step Up Together edition of Intermittent Auscultation Simulation-Based Education—a virtual course designed for nurses, midwives, paramedics, physicians, and other clinical team members committed to providing safe, patient-centered care during labor.

Proven, Practical Training for Perinatal Teams
Originally developed by Step Up Together founder Amy Romano and perinatal quality leader Debra Bingham, this first-of-its-kind course has equipped thousands of learners with essential fetal assessment skills. Now available to the Step Up Together community, this interactive, self-paced program combines simulation, competency assessment, and real-world application to close training gaps and standardize IA education.
What's Included?
Course Outline
Frequently asked questions
Why should perinatal practitioners learn intermittent auscultation?
Evidence supports use of intermittent auscultation (IA) instead of continuous electronic fetal monitoring in low-risk labor. IA supports freedom of movement and may help reduce the risk of cesarean or operative vaginal birth. Education and opportunities to practice IA skills are necessary to ensure IA is performed reliably, safely, and consistently.
How does the simulation work?
The program includes two didactic sections with comprehension quiz questions and a simulation module with skill check questions. The simulations show a video of an animated laboring woman in a birth room with an audio track of a fetal heart rate. Visual and audio cues are given to help the learner distinguish when the contraction is beginning, peaking, going away, and completely gone. The video includes a full contraction cycle from the beginning of one contraction to just before the beginning of the next. The learner listens and counts the rate, then responds to questions about the baseline, presence or absence of accelerations and decelerations, category (I or II), and plan of care. Case information and instructions are provided to assist the learner to prepare for, perform, and interpret the simulation.
Is the program designed for hospital birth or is it also appropriate for community settings (freestanding birth center/home)?
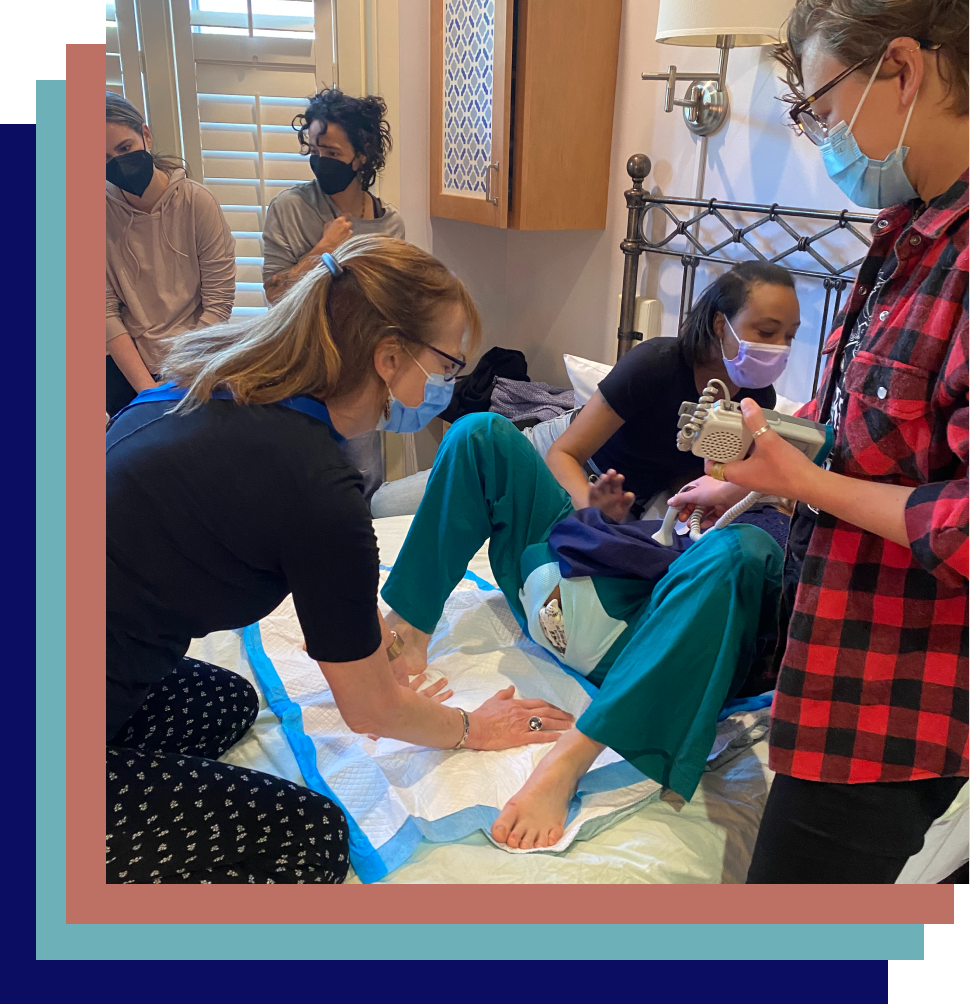
The program is appropriate for all birth settings, and includes imagery of IA taking place in hospital, birth center, and home births.
Who is the intended audience for the program?
The education program is appropriate for perinatal nurses, midwives, and physicians who provide intrapartum care, as well as students/clinical learners in these specialties.
Which IA methods and terminology does the program teach, and what is the evidence to support this approach?
There is not strong evidence to recommend any specific method or approach to intermittent auscultation. The program teaches the same approach that is recommended in Fetal Heart Monitoring: Principles and Practice (6th Edition), published by AWHONN and is consistent with Consensus Guidelines for Intermittent Auscultation in Community Birth Settings developed for community (home and birth center) midwifery practice. These include:
AWHONN recommends that facilities determine their own guidelines for frequency of auscultation. The program presents the range of professional guidelines from AWHONN, ACOG, ACNM, and the Community Birth consensus guidelines: Listening on admission, every 1-2 hours in early/latent labor (if admitted or being clinically observed), every 15-30 minutes in first stage, and every 5-15 minutes in second stage.
- Using a Doppler device, rather than the electronic fetal monitor or a fetoscope, to perform IA
- Assessing and documenting baseline as a single average rate, by listening for two minutes within a 10 minute period in 30-60 second intervals, between contractions when the fetus is not moving
- Assessing for and documenting accelerations and decelerations, though not the type of decelerations/decreases detected (e.g. early, variable, late).
- Categorizing fetal assessment as Category I or Category II based on baseline rate and rhythm and presence or absence of decelerations
- If Category II based on IA findings, changing maternal position and increasing frequency of auscultation or considering a 20-minute continuous fetal monitoring strip.
AWHONN recommends that facilities determine their own guidelines for frequency of auscultation. The program presents the range of professional guidelines from AWHONN, ACOG, ACNM, and the Community Birth consensus guidelines: Listening on admission, every 1-2 hours in early/latent labor (if admitted or being clinically observed), every 15-30 minutes in first stage, and every 5-15 minutes in second stage.
